Preventive pediatrics
Preventive Pediatrics
Comprehensive Nursing Notes
Table of Contents
1. Concept of Preventive Pediatrics
Definition and Importance
Preventive Pediatrics refers to the branch of medicine that focuses on preventing diseases, injuries, and promoting optimal health and development in children from birth through adolescence. It encompasses a range of interventions that aim to protect, promote, and maintain the health and well-being of children before diseases or conditions develop.
Core Principle:
"Prevention is better than cure" is the fundamental principle that guides preventive pediatrics, emphasizing proactive health measures rather than reactive treatment.
Primary Prevention
Measures taken to prevent the onset of disease by removing causes or risk factors
Examples: Immunization, nutritional counseling, safety education
Secondary Prevention
Early detection and intervention to halt disease progression
Examples: Screening programs, growth monitoring, developmental assessments
Tertiary Prevention
Management of established disease to prevent complications and disability
Examples: Rehabilitation services, management of chronic conditions
Key Components of Preventive Pediatrics
Preventive Pediatrics Mind Map
Growth & Development Monitoring
Immunization
Nutrition
Disease Prevention
Injury Prevention
Mental Health
1. Growth and Development Monitoring
- Regular assessment of height, weight, and head circumference
- Developmental milestone tracking
- Early identification of developmental delays or abnormalities
- Regular health check-ups and well-child visits
2. Nutrition
- Promotion of breastfeeding
- Age-appropriate complementary feeding guidance
- Prevention of micronutrient deficiencies
- Healthy eating habits and prevention of childhood obesity
3. Immunization
- Administration of vaccines according to recommended schedules
- Education on vaccine-preventable diseases
- Monitoring of adverse events following immunization
4. Disease Prevention
- Prevention of infectious diseases through hygiene practices
- Screening for genetic and congenital disorders
- Environmental health considerations
5. Injury Prevention
- Child safety education
- Prevention of accidents and injuries
- Safe home and play environment guidance
6. Mental Health
- Early identification of behavioral and emotional issues
- Promotion of positive parenting practices
- Prevention of adverse childhood experiences
Nursing Insight:
Preventive pediatric care is most effective when delivered through a multidisciplinary approach, with nurses playing a crucial role in health promotion, education, screening, and connecting families with appropriate resources. The nurse's consistent presence throughout a child's healthcare journey provides continuity that strengthens preventive efforts.
Role of Nurses in Preventive Pediatrics
| Role | Key Responsibilities | Impact on Child Health |
|---|---|---|
| Health Educator |
|
Empowers families with knowledge to make informed health decisions |
| Immunization Provider |
|
Protects children from vaccine-preventable diseases |
| Growth & Development Monitor |
|
Enables early intervention for growth/developmental issues |
| Health Screener |
|
Facilitates early detection and treatment of health problems |
| Advocate |
|
Ensures children receive necessary healthcare services |
| Case Manager |
|
Provides comprehensive support for complex health needs |
Mnemonic: "SHIELD" for Nursing Role in Preventive Pediatrics
S - Screening and surveillance of health status
H - Health education for families and communities
I - Immunization administration and monitoring
E - Early intervention for identified risks
L - Liaison between healthcare services and families
D - Documentation and follow-up of preventive care
2. Immunization
Fundamentals of Immunization
Immunization is the process of inducing immunity artificially by administering an immunobiologic agent. It is one of the most cost-effective and successful public health interventions, preventing millions of childhood illnesses, disabilities, and deaths from infectious diseases worldwide.
Active Immunization
Stimulates the body's immune system to produce its own antibodies against specific pathogens
Examples: Most routine childhood vaccines (MMR, DTaP, Polio vaccines)
Duration: Usually provides long-lasting immunity (years to lifetime)
Passive Immunization
Provides temporary immunity through antibodies produced outside the body
Examples: Immunoglobulins, maternal antibodies to newborn
Duration: Short-term protection (weeks to months)
Key Concept:
Herd immunity (community immunity) occurs when a sufficient portion of the population is immune to an infectious disease, making its spread from person to person unlikely. This indirectly protects those who cannot be vaccinated, such as infants, pregnant women, or immunocompromised individuals.
Types of Vaccines
| Vaccine Type | Composition | Examples | Special Considerations |
|---|---|---|---|
| Live Attenuated | Weakened form of the live virus or bacteria | MMR, Varicella, Rotavirus, Oral polio (OPV), BCG |
|
| Inactivated/Killed | Killed virus or bacteria | IPV (Inactivated Polio), Hepatitis A, Pertussis |
|
| Toxoid | Inactivated toxins from bacteria | Tetanus, Diphtheria |
|
| Subunit/Recombinant | Specific pieces of the pathogen | Hepatitis B, HPV, Acellular pertussis |
|
| Conjugate | Combines weak antigen with protein carrier | Hib, Pneumococcal conjugate, Meningococcal |
|
| mRNA | Messenger RNA that instructs cells to produce viral proteins | Some COVID-19 vaccines |
|
Mnemonic: "LIMITS" for Vaccine Types
L - Live attenuated (MMR, Varicella)
I - Inactivated whole agent (IPV)
M - mRNA vaccines (newer technology)
I - Immunoglobulins (passive immunity)
T - Toxoids (Tetanus, Diphtheria)
S - Subunit and conjugate vaccines
Recommended Immunization Schedule
The immunization schedule varies by country based on local epidemiology, available resources, and health priorities. The following represents a general guideline based on WHO recommendations:
Childhood Immunization Schedule
| Age | Recommended Vaccines |
|---|---|
| Birth | BCG, Hepatitis B (first dose), OPV (birth dose) |
| 6 weeks | DTaP/DTP (1st), Hepatitis B (2nd), Hib (1st), IPV/OPV (1st), Rotavirus (1st), PCV (1st) |
| 10 weeks | DTaP/DTP (2nd), Hib (2nd), IPV/OPV (2nd), Rotavirus (2nd), PCV (2nd) |
| 14 weeks | DTaP/DTP (3rd), Hepatitis B (3rd), Hib (3rd), IPV/OPV (3rd), Rotavirus (3rd), PCV (3rd) |
| 9 months | Measles (1st) or MMR (1st), Vitamin A |
| 12-15 months | MMR (1st if not given earlier), Varicella (1st), PCV (booster), Hepatitis A (1st) |
| 15-18 months | DTaP/DTP (4th), Hib (booster), IPV (booster) |
| 18-24 months | Hepatitis A (2nd) |
| 4-6 years | DTaP/DTP (5th), IPV (booster), MMR (2nd), Varicella (2nd) |
| 9-14 years | HPV (2 doses, 6 months apart) |
| 10-12 years | Tdap booster, Meningococcal conjugate |
Key:
BCG: Bacillus Calmette-Guérin (tuberculosis vaccine)
DTaP/DTP: Diphtheria, Tetanus, acellular Pertussis/Diphtheria, Tetanus, Pertussis
Hib: Haemophilus influenzae type b
HPV: Human Papillomavirus
IPV/OPV: Inactivated Polio Vaccine/Oral Polio Vaccine
MMR: Measles, Mumps, Rubella
PCV: Pneumococcal Conjugate Vaccine
Tdap: Tetanus, diphtheria, acellular pertussis (adolescent/adult formulation)
Important Note:
Always refer to your country's current national immunization schedule, as recommendations may vary. Special considerations may apply for children with certain medical conditions, premature infants, or during disease outbreaks.
Contraindications and Precautions
True Contraindications
- Severe allergic reaction (anaphylaxis) to a previous dose of vaccine or vaccine component
- Severe immunodeficiency for live vaccines
- Pregnancy for certain live vaccines (MMR, Varicella)
- Encephalopathy within 7 days of previous dose of pertussis-containing vaccine
Precautions (Requires Clinical Assessment)
- Moderate to severe acute illness with or without fever
- Recent receipt of antibody-containing blood products
- History of Guillain-Barré syndrome within 6 weeks of previous vaccine dose
- Unstable neurological conditions
- Family history of seizures for pertussis-containing vaccines
Nursing Consideration:
Many conditions are often mistakenly considered contraindications but are NOT true contraindications to vaccination:
- Mild acute illness with low-grade fever
- Current antimicrobial therapy
- Convalescent phase of illness
- Premature birth (for most vaccines)
- Recent exposure to infectious disease
- Family history of adverse reactions to vaccines
Adverse Events Following Immunization (AEFI)
Adverse Events Following Immunization (AEFI) are any untoward medical occurrences that follow immunization but do not necessarily have a causal relationship with the vaccine. Monitoring, reporting, and managing AEFIs is an essential component of immunization safety surveillance.
| Classification | Description | Examples | Nursing Management |
|---|---|---|---|
| Mild/Common Reactions | Expected, self-limiting reactions |
|
|
| Moderate to Severe | Less common but significant reactions |
|
|
| Serious | Rare, life-threatening reactions |
|
|
Anaphylaxis Management Protocol
- Position patient flat (or semi-reclining if respiratory distress), do not stand or sit them up
- Call for emergency medical assistance
- Administer epinephrine 1:1000 (0.01 mg/kg, max 0.5 mg) IM into anterolateral thigh
- Monitor vital signs (pulse, respiration, blood pressure)
- Provide oxygen if available
- Establish IV access if possible
- Repeat epinephrine every 5-15 minutes if needed
- Consider secondary medications (antihistamines, corticosteroids) after epinephrine
AEFI Reporting
Critical information to document and report:
- Patient demographics
- Vaccine details (name, manufacturer, lot number, expiration date)
- Date, time, and site of administration
- Onset, nature, and duration of adverse event
- Treatment provided and outcome
- Relevant medical history
- Previous vaccine reactions
Nursing Responsibilities in Immunization
Nursing Process in Immunization
Before Immunization
- Review child's immunization history
- Screen for contraindications and precautions
- Provide Vaccine Information Statements (VIS)
- Obtain informed consent from parents/guardians
- Address parental concerns and misconceptions
- Prepare vaccines properly according to manufacturer guidelines
- Check the "5 Rights" of medication administration
During Immunization
- Position child appropriately for comfort and safety
- Use age-appropriate distraction techniques
- Select appropriate needle size and injection site
- Follow correct administration technique
- Maintain aseptic technique throughout
- Properly dispose of used supplies in sharps containers
After Immunization
- Monitor child for 15-30 minutes for immediate adverse reactions
- Document vaccine details in child's health record and immunization card
- Educate parents about expected reactions and when to seek medical attention
- Provide instructions for managing common side effects
- Schedule next immunization visit
- Report any adverse events through appropriate channels
Mnemonic: "VACCINATE" for Nursing Responsibilities
V - Verify patient identity and vaccine history
A - Assess for contraindications and precautions
C - Comfort measures and positioning
C - Correct technique for administration
I - Inform parents about benefits and risks
N - Note details in immunization records
A - Adverse reaction monitoring and management
T - Teach about expected reactions and care
E - Ensure follow-up appointment scheduling
3. Immunization Programs and Cold Chain
National Immunization Programs
National Immunization Programs (NIPs) are comprehensive health initiatives designed to prevent vaccine-preventable diseases through systematic vaccination of target populations. These programs are typically government-led and aim to achieve high vaccination coverage to protect individuals and communities.
Key Components of NIPs
- Policy development and strategic planning
- Financial sustainability and resource allocation
- Vaccine procurement and supply chain management
- Service delivery and accessibility
- Healthcare worker training and supervision
- Program monitoring and evaluation
- Communication and community engagement
- Disease surveillance and outbreak response
Common Challenges in NIPs
- Vaccine hesitancy and misinformation
- Reaching underserved populations
- Cold chain maintenance in resource-limited settings
- Ensuring sustainable funding
- Staffing shortages and training needs
- Integration with other health services
- Monitoring adverse events
- Adapting to changing epidemiology
Global Initiative:
The Expanded Programme on Immunization (EPI) was established by the World Health Organization (WHO) in 1974 to develop and expand immunization programs worldwide. The initial EPI vaccines included BCG, DTP, OPV, and measles. Today, most countries have adopted and expanded the EPI to include additional vaccines based on their specific disease burden and resources.
Service Delivery Strategies
| Strategy | Description | Advantages | Challenges |
|---|---|---|---|
| Fixed Site Immunization | Routine immunization services provided at healthcare facilities |
|
|
| Outreach Services | Healthcare workers travel to provide services in semi-permanent facilities in underserved areas |
|
|
| Mobile Strategies | Mobile teams visit communities with no health facilities or difficult access |
|
|
| Supplementary Immunization Activities (SIAs) | Mass vaccination campaigns targeting specific populations or diseases |
|
|
| School-Based Immunization | Vaccination provided in schools to reach school-aged children |
|
|
Nursing Insight:
Successful immunization programs typically use a combination of delivery strategies to achieve optimal coverage. Nurses should be versatile in adapting to different service delivery contexts while maintaining standards for safe immunization practices.
Cold Chain System
The cold chain is a system of storage and transport procedures designed to maintain vaccines at appropriate temperatures from the point of manufacture to the point of administration. Maintaining the cold chain is critical for preserving vaccine potency and effectiveness.
The Vaccine Cold Chain System
Temperature Requirements
Frozen
-15°C to -25°C
- Oral polio vaccine (OPV) - for long-term storage
- Some varicella vaccines
- Some typhoid vaccines
Refrigerated
+2°C to +8°C
- Most routine vaccines (DTP, Hepatitis B, Hib, IPV, PCV, Rotavirus)
- OPV for short-term storage
- MMR, BCG
- Diluents (should be cooled before use)
Controlled Room Temperature
+15°C to +25°C
- Most diluents (when stored separately)
- Some vaccines in VVM category 4 during immunization sessions
Cold Chain Equipment
- Cold rooms: Large-scale storage at national/regional levels
- Freezers: For storing frozen vaccines and making ice packs
- Refrigerators: For storing vaccines at +2°C to +8°C
- Compression refrigerators (electric)
- Absorption refrigerators (gas/kerosene)
- Solar refrigerators
- Ice-lined refrigerators
- Cold boxes: Insulated containers for vaccine transport (1-7 days)
- Vaccine carriers: Smaller portable insulated containers (1-2 days)
- Ice packs: For keeping cold boxes and vaccine carriers cold
- Temperature monitoring devices: Thermometers, temperature loggers, VVM
Vaccine Vial Monitor (VVM)
A VVM is a heat-sensitive label attached to vaccine vials that changes color when the vaccine has been exposed to heat over time, indicating potential reduction in potency.
Stage 1: Use the vaccine
Stage 2: Use the vaccine
Stage 3: Use if inner square lighter than outer ring
Stage 4: Discard the vaccine
Maintaining the Cold Chain: Best Practices
Storage Guidelines
- Store vaccines according to manufacturer recommendations
- Arrange vaccines to allow air circulation
- Keep freeze-sensitive vaccines away from freezer walls or ice packs
- Store vaccines with the earliest expiry dates in front
- Never store vaccines in refrigerator doors
- Maintain stock records and conduct regular inventory
- Keep diluents with their corresponding vaccines
Temperature Monitoring
- Monitor and record temperatures twice daily (morning and evening)
- Use temperature monitoring devices appropriately
- Take immediate action if temperatures fall outside recommended range
- Have a contingency plan for power outages or equipment failure
- Conduct regular maintenance of cold chain equipment
Mnemonic: "COLD CHAIN" for Cold Chain Management
C - Check temperatures twice daily
O - Organize vaccines properly in storage
L - Label clearly with expiry dates
D - Document temperature readings
C - Contingency plans for emergencies
H - Handle vaccines with care during transport
A - Assess VVMs before vaccine use
I - Inventory management (FEFO - First Expiry, First Out)
N - Never freeze freeze-sensitive vaccines
Critical Alert:
Vaccines exposed to temperatures outside their recommended range may lose potency and provide inadequate protection. Always follow proper storage procedures and never administer vaccines if their cold chain integrity is compromised. When in doubt, consult supervisors before using potentially compromised vaccines.
Nursing Responsibilities in Immunization Programs
Program Planning & Management
- Participate in microplanning for immunization services
- Help identify target populations and hard-to-reach groups
- Assist in vaccine forecasting and stock management
- Support monitoring and evaluation activities
- Maintain accurate records and reporting systems
- Participate in coverage assessments
Cold Chain Management
- Monitor refrigerator temperatures regularly
- Organize vaccines appropriately in storage
- Prepare and condition ice packs correctly
- Pack and transport vaccines safely
- Identify and report cold chain problems
- Implement contingency plans for cold chain failures
- Check VVMs before using vaccines
Community Engagement
- Conduct community outreach and education
- Address vaccine hesitancy and misinformation
- Collaborate with community leaders and influencers
- Track and follow up with defaulters
- Engage in social mobilization activities
- Provide education on vaccine-preventable diseases
- Create supportive environment for immunization
Nursing Leadership in Immunization Programs:
Nurses often serve as the backbone of immunization programs, particularly at the service delivery level. Beyond technical skills, nurses contribute significantly through their leadership, problem-solving abilities, and trusted relationships with communities. Advanced practice nurses may also participate in program design, policy development, and research to improve immunization services.
Monitoring and Evaluation
Effective monitoring and evaluation (M&E) are essential for assessing immunization program performance, identifying gaps, and guiding improvements. Nurses are critical participants in data collection, analysis, and using data for decision-making at the facility level.
| Key Indicators | Description | Calculation | Target |
|---|---|---|---|
| Immunization Coverage | Percentage of target population that received a specific vaccine | (Number of individuals receiving specific vaccine ÷ Target population) × 100 | ≥90% national, ≥80% in all districts |
| Dropout Rate | Percentage of children who started but did not complete a vaccination series | [(First dose - Last dose) ÷ First dose] × 100 | <10% |
| Vaccine Wastage Rate | Percentage of vaccine doses discarded without being administered | [(Doses used - Doses administered) ÷ Doses used] × 100 | Varies by vaccine, generally <25% |
| Adverse Events Following Immunization (AEFI) Rate | Rate of adverse events per number of doses administered | (Number of specific AEFIs ÷ Number of doses administered) × 1000 or 10,000 | Varies by vaccine and event type |
| Cold Chain Integrity | Percentage of time temperature stays within recommended range | (Number of temperature recordings within range ÷ Total number of recordings) × 100 | 100% |
| Vaccine Availability | Percentage of days vaccine was available without stockout | (Number of days without stockout ÷ Total number of days) × 100 | 100% |
Data Collection Tools
- Immunization registers
- Tally sheets
- Child health/immunization cards
- Stock management records
- Temperature monitoring logs
- AEFI reporting forms
- Supervisory checklists
- Electronic immunization registries (where available)
Using Data for Action
- Conduct regular data reviews at facility level
- Identify children who missed vaccines (defaulter tracking)
- Monitor coverage trends to identify underperforming areas
- Analyze dropout rates to improve retention
- Review cold chain data to ensure vaccine quality
- Plan outreach services based on coverage gaps
- Adjust stock management practices based on wastage data
- Investigate and respond to adverse events
Data Quality:
The reliability of monitoring and evaluation depends heavily on data quality. Nurses should ensure that immunization data is complete, accurate, consistent, and timely. Regular data verification exercises can help identify and correct issues with data recording and reporting. Remember: "Poor data leads to poor decisions, good data enables good decisions."
Summary and Key Points
Preventive Pediatrics
- Focuses on preventing diseases and promoting optimal child health
- Encompasses primary, secondary, and tertiary prevention
- Nurses play crucial roles in assessment, education, and advocacy
- Addresses physical, developmental, and psychosocial aspects of health
Immunization
- One of the most effective public health interventions
- Various vaccine types provide active immunity against diseases
- Safe administration requires proper technique and precautions
- Nurses must understand contraindications and manage adverse events
Immunization Programs & Cold Chain
- National programs coordinate comprehensive vaccination services
- Multiple delivery strategies reach diverse populations
- Cold chain system ensures vaccine potency from manufacture to use
- Monitoring and evaluation guide program improvements
Final Thoughts for Nursing Students
As a nurse working in preventive pediatrics, you will be at the forefront of protecting children's health and building foundations for lifelong wellness. Your knowledge, skills, and compassion will directly impact vaccination coverage, disease prevention, and health promotion in your community.
Remember that immunization is not just a technical procedure but an opportunity for holistic care—to assess a child's overall health, educate families, address concerns, and build trusting relationships. By mastering the concepts in these notes and applying them with care and cultural sensitivity, you will contribute significantly to reducing childhood morbidity and mortality from preventable diseases.
References and Further Reading
- World Health Organization. (2020). Immunization Agenda 2030: A Global Strategy to Leave No One Behind.
- Centers for Disease Control and Prevention. (2023). Pink Book: Epidemiology and Prevention of Vaccine-Preventable Diseases.
- American Academy of Pediatrics. (2021). Red Book: Report of the Committee on Infectious Diseases.
- World Health Organization. (2018). Immunization in Practice: A practical guide for health staff.
- World Health Organization. (2015). Immunization in Practice, Module 3: The Cold Chain.
- UNICEF & WHO. (2019). Guidance on the monitoring and surveillance of COVID-19 vaccination programmes.
- World Health Organization. (2019). Immunization Supply Chain and Logistics: A neglected but essential system for national immunization programmes.
- Plotkin, S., Orenstein, W., Offit, P., & Edwards, K. M. (2018). Plotkin's Vaccines (7th ed.). Elsevier.
Care of Under-Five and Well-Baby Clinics
Comprehensive Nursing Notes
Table of Contents
- 1. Introduction
- 2. Under-Five Clinics
- 3. Well-Baby Clinics
- 4. Growth Monitoring
- 5. Immunization Schedules
- 6. Preventive Measures for Accidents
- 7. Role of Nurses
- 8. References
Introduction
The first five years of life form the foundation of a child's physical, cognitive, and emotional development. During this critical period, children are most vulnerable to health issues and injuries, making it essential to provide comprehensive healthcare services targeted specifically to this age group.
Under-five and well-baby clinics were designed to provide a comprehensive package of preventive, promotive, curative, and referral services to children under one roof. These clinics focus on:
- Regular growth and development monitoring
- Timely immunizations
- Early detection and management of health issues
- Prevention of common childhood accidents
- Health education for parents and caregivers
This comprehensive approach ensures that children receive holistic care that addresses all aspects of their health and development during these formative years.
Under-Five Clinics
Goal and Objectives
The overall goal of the under-five clinic is to provide comprehensive healthcare to young children in a specialized facility. The specific objectives include:
- Monitor growth and development of the child until 5 years of age
- Identify factors that may hinder the growth and development of the child
- Provide timely interventions for health issues
- Ensure complete immunization coverage
- Educate caregivers on proper childcare practices
Symbol of Under-Five Clinic
Fig. 1: Symbol of Under-Five Clinic showing five components of care
Key Activities and Services
G - Growth monitoring
O - Oral rehydration therapy
P - Preventive care (immunizations, nutrition)
H - Health education for parents
E - Examination and treatment of illnesses
R - Referral of complex cases
1. Care in Illness
Children are treated for acute and chronic illnesses and ailments related to growth and development. This includes:
- Diagnosis and treatment of common childhood illnesses
- X-ray and laboratory services
- Referral services for complex cases
2. Growth Monitoring
This is one of the most important functions of the clinic. The monitoring schedule includes:
- Monthly weighing during the first year
- Every 2 months from 1 to 3 years of age
- Every 3 months in 4th and 5th years
Besides weighing, measuring height and mid-arm circumference are also carried out. Growth is plotted on growth charts to monitor the child's progress.
3. Preventive Care
This includes:
- Timely physical examination of children
- Immunization according to national schedule
- Nutritional care:
- Surveillance on food supplementation
- Health check-ups every 3-6 months
- Management of nutrition among newborns and children
- Oral rehydration therapy for diarrheal diseases
4. Family Planning
Family planning is central to any program directed towards women and children. The clinic:
- Educates people on contraceptive methods
- Provides health education on family planning and birth spacing
- Offers psychological support to mothers
5. Health Education
The clinic educates mothers about:
- Child care practices
- Breastfeeding and complementary feeding
- Nutrition and growth monitoring
- Immunization importance and schedule
- Cleanliness and hygiene practices
Well-Baby Clinics
Age Groups Covered
Well-baby clinics focus on children from birth to under 6 years old, divided into:
- Infancy (up to one year)
- Preschool age (1 year to 6 years)
Importance of Well-Baby Clinics
- Child health care is a crucial element of primary health care
- Children represent about 15% of the total population
- Children are more susceptible to high mortality
- They are more vulnerable and need proper monitoring of growth and development
- Early detection and management of preventable and treatable diseases is essential
- High-quality healthcare for babies leads to healthier communities
Well-Baby Clinic Services Mind Map
Objectives of Well-Baby Clinics
- Provide comprehensive health education to parents
- Ensure adequate nutrition for optimal growth
- Administer complete immunization according to schedule
- Provide care during illness
- Offer rehabilitation services when necessary
Schedule of Well-Baby Clinic Visits
| Age | Number of Visits | Timing of Visits |
|---|---|---|
| First Year | 6 visits | After delivery, 2 months, 4 months, 6 months, 9 months, and 12 months |
| After One Year | 7 visits | 1.5 years, 2 years, 2.5 years, 3 years, 3.5 years, 4 years, and 4.5 years |
Components of Well-Baby Clinics
1. Resources and Structures (Manpower)
- Trained physicians
- Trained female nurse-midwives
- Support staff with appropriate qualifications
2. Examinations and Procedures
- Anthropometric measurements:
- Weight, height, head circumference
- Temperature measurement
- General appearance assessment
- Physical examination of:
- Fontanels, ears (hearing defect, otitis media)
- Eyes (squint and glaucoma)
- Lips (anemia and cleft palate)
- Muscles and genitalia
- Developmental assessment:
- Muscle tone
- Developmental milestones according to age
- Reflexes
3. Immunization Services
One of the most important services offered by well-baby clinics is the provision of immunizations for childhood diseases such as:
- Diphtheria, Pertussis, Tetanus (DPT)
- Polio
- Haemophilus influenzae type b
- Hepatitis B
- Measles, Mumps, Rubella
- Varicella (Chickenpox)
Growth Monitoring
Importance of Growth Monitoring
- Early detection of growth faltering or excessive growth
- Identification of underlying health conditions
- Assessment of nutritional status
- Evaluation of response to interventions
- Projection of adult height
Growth Monitoring Schedule
| Age | Frequency | Parameters Measured |
|---|---|---|
| 0-1 year | Monthly | Weight, Length, Head Circumference |
| 1-3 years | Every 2 months | Weight, Height, Head Circumference (up to 2 years) |
| 3-5 years | Every 3 months | Weight, Height |
Growth Charts
The World Health Organization (WHO) growth standards are used globally for monitoring child growth. These charts represent how children should grow under optimal conditions and are considered the gold standard for assessing growth worldwide.
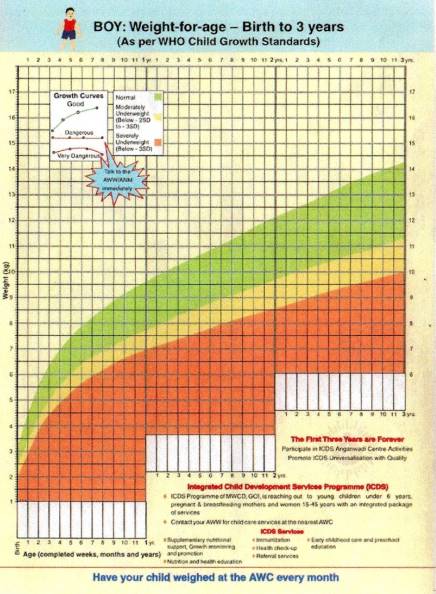
Fig. 2: WHO Growth Chart for Boys (0-5 years)
How to Use Growth Charts
- Measure accurately: Use standardized equipment and proper technique
- Plot measurements: Mark the child's measurements on the appropriate chart according to age and gender
- Connect the dots: Draw a line connecting previous and current measurements to form a growth curve
- Interpret the curve: Compare the child's growth curve with the standard curves on the chart
- Identify growth issues: Look for deviations from the expected pattern
P - Position on the chart (percentile)
L - Look at previous measurements (pattern)
O - Observe for crossing percentile lines
T - Trends over time (upward, flat, or downward)
S - Sudden changes (require immediate attention)
Interpreting Growth Patterns
| Growth Pattern | Interpretation | Potential Causes |
|---|---|---|
| Normal growth | Growth curve parallels the standard curves | Adequate nutrition and health |
| Growth faltering | Flattening or downward trend of the growth curve | Inadequate nutrition, infection, chronic illness |
| Catch-up growth | Upward crossing of percentile lines | Recovery from illness, improved nutrition |
| Excessive growth | Upward crossing of multiple percentile lines | Overfeeding, endocrine disorders |
Interventions for Growth Issues
- Growth faltering:
- Nutritional counseling and supplementation
- Treatment of underlying infections
- More frequent monitoring
- Excessive weight gain:
- Dietary assessment and modification
- Promotion of physical activity
- Screening for endocrine disorders
- Abnormal head growth:
- Evaluation for hydrocephalus or microcephaly
- Neurological assessment
- Referral to specialist
Immunization Schedules
Immunization is one of the most cost-effective public health interventions, preventing millions of deaths and disabilities worldwide. Following the recommended schedule ensures children receive optimal protection at the appropriate ages.
Recommended Childhood Immunization Schedule (0-5 years)
| Age | Vaccines | Notes |
|---|---|---|
| Birth | Hepatitis B (1st dose), BCG | HepB should be given within 24 hours of birth |
| 6 weeks | DTaP/DPT (1st dose), IPV (1st dose), Hib (1st dose), PCV (1st dose), Rotavirus (1st dose), Hepatitis B (2nd dose) | Start of primary series |
| 10 weeks | DTaP/DPT (2nd dose), IPV (2nd dose), Hib (2nd dose), PCV (2nd dose), Rotavirus (2nd dose) | Continuation of primary series |
| 14 weeks | DTaP/DPT (3rd dose), IPV (3rd dose), Hib (3rd dose), PCV (3rd dose), Rotavirus (3rd dose), Hepatitis B (3rd dose) | Completion of primary series |
| 9 months | Measles (1st dose), Yellow Fever (in endemic areas) | Early protection against measles |
| 12-15 months | MMR (1st dose), Varicella (1st dose), PCV (booster), Hib (booster) | First dose of MMR and varicella |
| 15-18 months | DTaP/DPT (1st booster), IPV (booster) | First boosters for DTaP and IPV |
| 4-6 years | DTaP/DPT (2nd booster), IPV (booster), MMR (2nd dose), Varicella (2nd dose) | School entry boosters |
Key Vaccines and Their Diseases
D - Diphtheria
I - Influenza
A - Acellular pertussis (whooping cough)
M - Measles
O - Oral Polio Vaccine
N - Neisseria meningitidis (meningococcal)
D - DTP (combined vaccine)
P - Pneumococcal
Ro - Rotavirus
V - Varicella (chickenpox)
I - IPV (inactivated polio vaccine)
D - DTaP (combined vaccine)
e - extra protection with boosters
H - Haemophilus influenzae type b
E - Encephalitis (Japanese, in endemic areas)
P - Hepatitis (A and B)
Common Side Effects and Management
| Side Effect | Associated Vaccines | Management |
|---|---|---|
| Fever | Most vaccines, especially DTaP, PCV, MMR | Paracetamol/Acetaminophen as needed; Encourage fluids |
| Local reactions (pain, redness, swelling) | All injectable vaccines | Cold compress; Paracetamol/Acetaminophen if needed |
| Irritability | Most vaccines | Comfort measures; Extra holding and cuddling |
| Rash | MMR, Varicella | Usually self-limiting; Calamine lotion if itchy |
| Drowsiness | Most vaccines | Allow extra rest |
Contraindications and Precautions
- General contraindications:
- Severe allergic reaction to a previous dose
- Known severe allergy to vaccine components
- Moderate to severe acute illness (temporary)
- Live vaccines (MMR, Varicella, Yellow Fever):
- Severe immunodeficiency
- Pregnancy
- Recent receipt of antibody-containing blood products
Preventive Measures for Accidents
Children are naturally curious and lack the judgment to recognize dangerous situations, making them particularly vulnerable to accidents. Preventive measures must be age-appropriate as different age groups face different risks.
Common Childhood Accidents Mind Map
Age-Specific Preventive Measures
1. Birth to 6 Months (Newborns)
| Risk Area | Preventive Measures |
|---|---|
| Transportation |
|
| Sleeping |
|
| Bathing/Water |
|
| Changing/Dressing |
|
| Choking Hazards |
|
2. 6 to 12 Months (Infants)
| Risk Area | Preventive Measures |
|---|---|
| Transportation |
|
| Water Safety |
|
| Feeding |
|
| Mobility |
|
3. 1 to 2 Years (Toddlers)
| Risk Area | Preventive Measures |
|---|---|
| Transportation |
|
| Water Safety |
|
| Dressing/Movement |
|
| Poisoning |
|
| Home Safety |
|
4. 2 to 5 Years (Early Childhood)
| Risk Area | Preventive Measures |
|---|---|
| Transportation |
|
| Water Safety |
|
| Burn Prevention |
|
| Mobility/Traffic |
|
| Sports/Activities |
|
General Safety Principles
S - Supervise children at all times
A - Age-appropriate environment and toys
F - Fasten and secure furniture, TVs, and appliances
E - Educate caregivers about potential hazards
K - Keep dangerous substances locked and out of reach
I - Install safety devices (gates, outlet covers, cabinet locks)
D - Develop and practice emergency plans
S - Safety equipment (car seats, helmets, life jackets) always used
Role of Nurses
Nurses play a pivotal role in under-five and well-baby clinics, serving as the frontline healthcare providers who often have the most consistent contact with children and their families. Their responsibilities span across all aspects of child healthcare.
Organization and Management
- Selection of appropriate location and scheduling of clinic days
- Arranging necessary equipment and supplies
- Setting up entertainment facilities for children
- Creating a warm, welcoming environment for mothers and children
- Proper record-keeping and documentation
Clinical Services
| Service Area | Nursing Responsibilities |
|---|---|
| Growth Monitoring |
|
| Immunization |
|
| Physical Assessment |
|
| Treatment and Management |
|
Health Education and Counseling
One of the most crucial roles of nurses in under-five and well-baby clinics is providing health education to parents and caregivers. This includes:
Nurse's Health Education Role Mind Map
Preventive Role in Accidents
Nurses play a vital role in preventing childhood accidents through:
- Educating parents about age-specific accident risks
- Demonstrating safety measures and proper use of safety equipment
- Conducting home safety assessments during home visits
- Providing anticipatory guidance as children reach new developmental stages
- Teaching first aid for common childhood injuries
- Advocating for safe community environments
Community Outreach
- Conducting home visits for high-risk families
- Tracking defaulters and encouraging clinic attendance
- Participating in community health campaigns
- Organizing health education sessions in community settings
- Facilitating mother support groups
- Coordinating with community leaders and organizations
C - Clinical assessment and care provision
A - Anthropometric measurements and growth monitoring
R - Record keeping and documentation
E - Education of parents and caregivers
4 - Four key areas: growth, development, nutrition, and safety
K - Knowledge dissemination about childcare practices
I - Immunization services provision
D - Detection of health problems early
S - Support for families through counseling and referral
References
- World Health Organization. (2023). WHO Growth Standards. https://www.who.int/tools/child-growth-standards/standards
- Centers for Disease Control and Prevention. (2024). Immunization Schedules. https://www.cdc.gov/vaccines/hcp/imz-schedules/index.html
- Rady Children's Hospital. (2023). Age-related Injury Prevention. https://www.rchsd.org/programs-services/center-for-healthier-communities/injury-prevention/age-related-injury-prevention/
- RNpedia. (2022). Under Five Clinic Program. https://www.rnpedia.com/nursing-notes/community-health-nursing-notes/five-clinic-program/
- Rama University. (2023). Under Five Clinics. https://www.ramauniversity.ac.in/online-study-material/nursing/gnm/2year/childhealthnursing/lecture-17.pdf
- UT Southwestern Medical Center. (2023). 5 common childhood injuries and how to prevent them. https://utswmed.org/medblog/childhood-injuries-prevention/
- Regis College. (2023). Child Injury Prevention: Common Childhood Injuries. https://online.regiscollege.edu/blog/preventing-childhood-injuries/
- Better Health Channel. (2023). Child safety and injury prevention. https://www.betterhealth.vic.gov.au/health/healthyliving/child-safety-and-injury-prevention
- Hong Kong Fire Services Department. (2022). Home Accident Prevention for Children. https://www.hkfsd.gov.hk/home/eng/source/safety/Children_home_accident.html
- American Academy of Pediatrics. (2024). All About the Recommended Immunization Schedules. https://www.healthychildren.org/English/safety-prevention/immunizations/Pages/Recommended-Immunization-Schedules.aspx
Comments
Post a Comment